Do you experience bloating, diarrhea, abdominal pain, or headaches after eating bread and other products containing wheat, barley, or rye? You could have a gluten intolerance, also known as non-celiac gluten sensitivity. Fortunately, gluten intolerance testing can help you pinpoint the problem.
Gluten Intolerance Testing
You can assess whether you have a gluten intolerance on your own at home, or you can have your healthcare professional order lab tests that will help you determine if gluten is a problem for you.
Gluten Intolerance Testing at Home
I have found the single best way to determine if you have an issue with gluten is with an elimination diet. This means you remove gluten from your diet for at least 30 days and then reintroduce it. Please note that gluten is a very large protein. It can take months or even years to completely clear from your system. The longer you can eliminate it from your diet before reintroducing it, the better.
Here’s the simple advice that I shared with all the patients in my clinic: If you feel significantly better when you’re not eating gluten and worse when you reintroduce it, then gluten is likely a problem for you. Remember, to get accurate results from this testing method you must eliminate 100% of the gluten from your diet.
Gluten Intolerance Testing at a Lab
Another way to determine if you are sensitive to gluten is to ask your doctor to order the following tests:
- IgA anti-gliadin antibodies (these are found in about 80% of people with Celiac disease)
- IgG anti-gliadin antibodies
- IgA anti-endomysial antibodies
- Tissue Transglutaminase antibodies
- Total IgA antibodies
- Genetic testing (HLA DQ2 and HLA DQ8)
- Intestinal biopsy (for celiacs)
A Potential Problem with Gluten Intolerance Testing
I want to mention that one potential problem with gluten intolerance testing is that gluten is made up of several hundred peptides and gliadin is made up of 12 different sub-fractions. Most modern-day gluten intolerance testing focuses on only the alpha-gliadin (one of the twelve sub-fractions.) Therefore, there is considerable room for error and false-negative tests.
However, a lab called Cyrex Lab tests for these sub-fractions and may help to minimize false negatives in gluten intolerance testing. Cyrex also offers an Array 4 test to check for gluten cross-reactivity with other grains.
The Key to Gluten Intolerance Testing
The key with these gluten intolerance test in the lab is you MUST be eating gluten (or other grains you are concerned about) for roughly 4 weeks prior to testing in order to detect gluten antibodies. That being said, if you know you don’t tolerate gluten I do not recommend adding it back into your diet just to see what happens on a test.
If you are certain that gluten is to blame for your symptoms, I would avoid it no matter what any test says! In my experience, testing does not always have the most valid responses when compared to the gold standard of an elimination diet.
As I often told the patents in my clinic: Your body knows better than any test. If your symptoms disappear when you take gluten out of your diet and return when you add it back in — even if you have a negative test result — you still have an issue with gluten. So don’t eat it
Celiac Disease Testing
I often get a lot of comments from readers when I write about giving gluten up for 30 days as part of a gluten sensitivity test. I want to be clear that I am not referring to celiac disease testing. The gold standard to diagnose celiac disease is still an intestinal biopsy. Identifying celiac disease is important because it is an autoimmune disease. Therefore, it can put you at risk for long-term complications if not properly addressed.
 Dr. Amy Myers
October 15th, 2018
https://content.amymyersmd.com/article/test-gluten-intolerance-celiac-disease/How Celiac Disease Affects Your Body – Infographic – Amy Myers MD®
Dr. Amy Myers
October 15th, 2018
https://content.amymyersmd.com/article/test-gluten-intolerance-celiac-disease/How Celiac Disease Affects Your Body – Infographic – Amy Myers MD®Symptoms of Celiac Disease
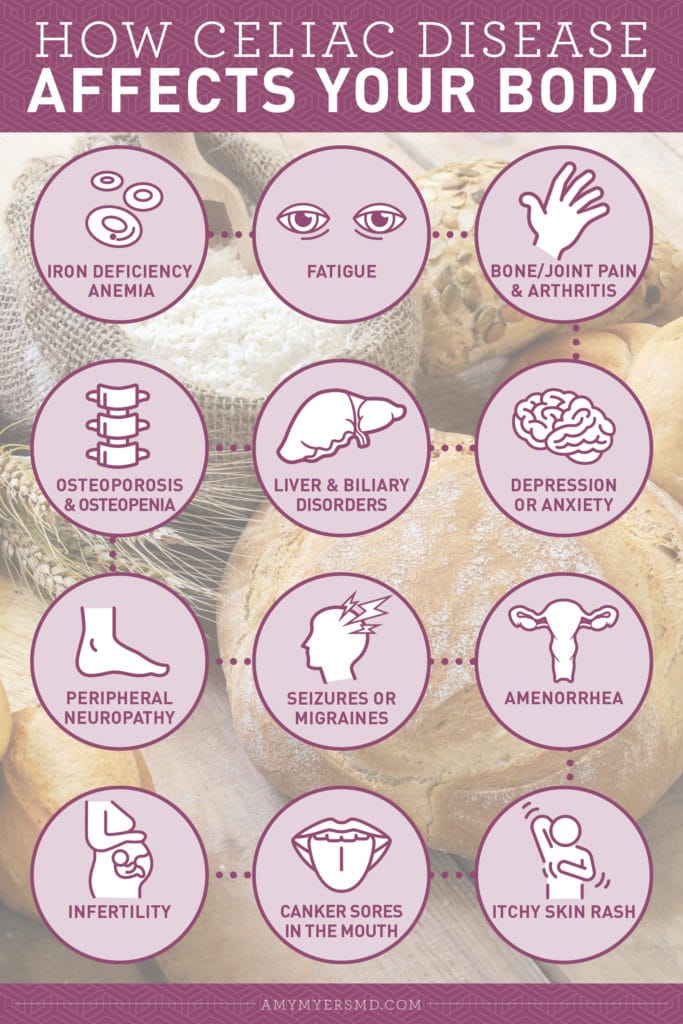
Although digestive issues are common in children with celiac disease, most adults do not experience these symptoms. Instead, the following signs are often a red flag for celiac disease in adults:
- Amenorrhea
- Arthritis
- Bone or joint pain
- Canker sores inside the mouth
- Depression or anxiety
- Fatigue
- Itchy skin rash1
- Infertility
- Liver and biliary tract disorders
- Osteoporosis or osteopenia
- Peripheral neuropathy (tingling, numbness, or pain in the hands and feet)
- Seizures or migraines
- Unexplained iron-deficiency anemia
Whether or not you are experiencing any of these symptoms, it is crucial to undergo celiac disease testing if you have a first-degree relative with the condition, as this puts you at a one in ten risk of developing celiac yourself.
However, if you suspect that you have gluten intolerance rather than celiac, the single best way gluten intolerance test is to remove it from your diet, note how you feel without it, and how you feel when you add it back in.
How to Treat Gluten Intolerance and Celiac Disease
Eliminating gluten from your diet means 100%. Even trace amounts of gluten from cross-contamination, medications, or supplements can be enough to cause an immune reaction in your body. The 80/20 rule; or “we don’t eat it in our house, just when we eat out” is a complete misconception.
A Lancet article published in 2001 states that for those with celiac disease or gluten sensitivity, eating gluten just once a month increased the relative risk of death by 600%.
The outward manifestation of eating gluten may be mild bloating or a headache. Inside your body, your immune system is being stimulated and the effects may last for three to six months.
For many, simply removing gluten completely from their diet isn’t enough. The damage that has been caused to the gut lining must also be repaired. Leaky Gut Revive™ can be a powerful ally in repairing your gut in conjunction with functional medicine’s 4R program.
Additionally, I often find that there are other infections in the gut that need to be addressed and corrected. Parasites, Candida overgrowth, small intestinal bacterial overgrowth (SIBO), and other imbalances can all be impacted by the cross-reactivity of gliadin sub-fractions in non-gluten grains.
When in doubt, go without. You’re not missing any vital nutrients by not eating gluten. In fact, you may well be improving your life dramatically!

