I talk a lot about autoimmunity. I first like to share the empowering news that genetics only accounts for about 25% of your risk of developing an autoimmune disease. That means 75% of your chance comes from external factors that you CAN impact, such as diet, toxins, infections, and stress.
Today, I want to focus on autoimmunity and infections –– specifically, the link between autoimmune conditions such as lupus and the human papillomavirus (HPV). While it may seem like infections just happen to us, in many cases, they are one of the root causes of autoimmunity that you absolutely can control.
What is Autoimmune Disease?
Autoimmune disease occurs when your body’s natural defense system can’t tell the difference between your own cells and foreign invaders, causing your body to mistakenly attack normal cells. The type of tissues that are being attacked determine which autoimmune condition will manifest.
If it’s the joints, rheumatoid arthritis can develop; with the thyroid gland, the result could affect thyroid hormones and lead to Hashimoto’s or Graves’ disease; in the gut lining itself, Crohn’s or colitis could develop. You can read more about autoimmune disease in my book, The Autoimmune Solution.
How Do You Get Lupus?
No one knows the exact trigger for any autoimmune condition, including lupus. At their core, all autoimmune diseases have one thing in common: chronic inflammation that causes your immune system to go rogue.
Just about any part of your body can be affected by lupus.
In the case of systemic lupus erythematosus or SLE, the most common type of lupus, just about any part of your body could be affected. Still, the chronic inflammation of SLE mostly affects the joints, skin, and internal organs. Symptoms vary from person to person, but most often, those with SLE experience pain and swelling of the joints. They may also develop skin rashes, sores, and mouth ulcers.
Over 1.5 million people in the United States have been diagnosed with SLE –– 90% of whom are women between the ages of 15-44. I’ll talk more about lupus and other autoimmune conditions in just a minute.1
What is the Human Papillomavirus (HPV)?
There are more than 100 varieties of human papillomavirus. Forty of them can infect the genitals, the anus, and the mouth. Those are the types I’ll discuss here. However, palmer warts (found on the hands) and plantar warts (found on the feet) are also caused by HPV strains.
HPV is generally divided into two types: low-risk and high-risk. The low-risk types of HPV are the ones that usually result in skin-colored warts in the oral, anal, or genital areas.2
The low-risk types, even those that are sexually transmitted, are usually completely harmless.
High-risk strains of HPV in women can lead to cervical cancer, cancer of the vulva, vagina, anus, mouth, and throat.3 In fact, HPV types 16 and 18 care responsible for up to 80% of all cervical cancers, the third most frequent cancer type in women.
Certain strains of HPV can lead to cancer.
In men, high-risk HPV strains can lead to cancers of the anus, mouth, and throat. Just like with the low-risk types, with the high-risk strains, you may never have HPV symptoms.
How Do You Get HPV?
All forms of HPV are transmitted by skin-to-skin contact. Sexually transmitted HPV can result from vaginal, anal, or oral sexual contact. The symptoms can develop years after you were initially infected.1
However, just like the types on your hands or feet, they often go away by themselves if you do develop symptoms. If your immune system is in optimal shape, your body can typically fight off the virus without you ever even knowing you had it.
That’s one of the reasons that HPV is the most common sexually transmitted infection. According to the Centers for Disease Control, about 79 million Americans have it.4
The other reason is that nearly all other STDS, such as gonorrhea and syphilis, are transferred by body fluid. Because HPV is simply transmitted through skin-to-skin contact,5it’s much easier to contract.
What’s the Relationship Between HPV and Autoimmunity?
Infection with HPV may also make you more susceptible to certain kinds of autoimmunity.
At the same time, autoimmunity may make you more susceptible to the virus and flares of it down the line.
 Dr. Amy Myers
October 11th, 2020
https://content.amymyersmd.com/article/hpv-and-autoimmunity/The Link Between HPV and Autoimmunity – Infographic – Amy Myers MD®
Dr. Amy Myers
October 11th, 2020
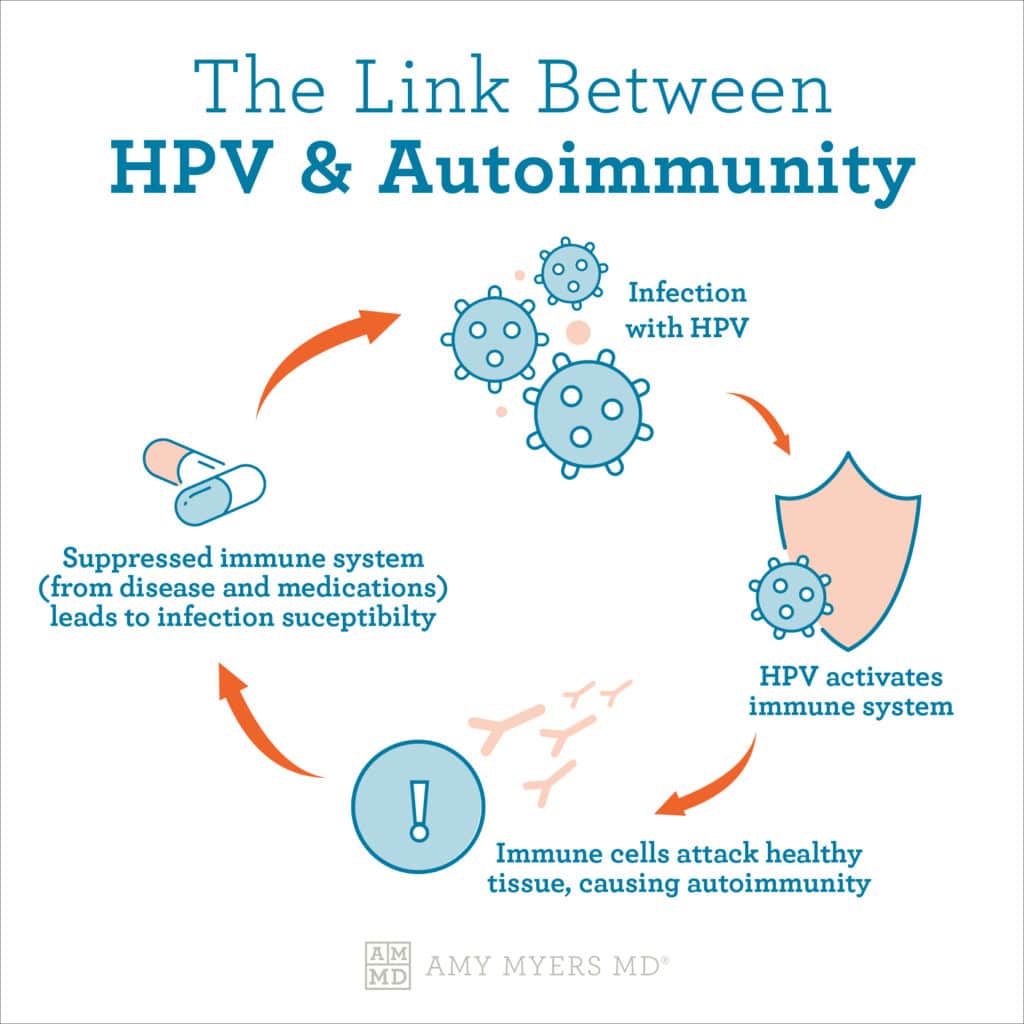
https://content.amymyersmd.com/article/hpv-and-autoimmunity/The Link Between HPV and Autoimmunity – Infographic – Amy Myers MD®HPV Can Lead to Autoimmunity
Infection with the HPV virus is linked to lupus as well as other autoimmune diseases including multiple sclerosis.6,7
It’s thought that the immune cells involved in certain autoimmune diseases may be the same as those activated during an immune response to certain types of HPV. So when you have HPV, your body unwittingly learns to attack healthy tissue, too, causing autoimmunity.8
For example, research shows that HPV infection is directly associated with the onset of several oral autoimmune diseases, including:
- oral lichen planus (OLP)
- mucous membrane pemphigoid (MMP)
- pemphigus vulgaris (PV)
- epidermolysis bullosa aquisita (EBA)9
Autoimmunity Can Lead to HPV
And you may be more likely to get infected with HPV if you already have autoimmunity. In addition, those with lupus are more likely to contract the HPV virus and to have cervical cancer than the general population of women.10
That’s because some immune system disorders cause abnormally low activity of the immune system, decreasing the body’s ability to fight invaders and therefore increasing vulnerability to infections.11
Viral infections never really go away; they can flare up when the body is under stress. However, this happens more persistently, and for more prolonged periods, in people with SLE. One study showed that for those without SLE, HPV cleared out within six months. However, 49% of those with SLE had persistent infection with HPV.12
Isn’t there a Vaccine to Prevent HPV Infection?
There are vaccines for HPV, yet they are not without controversy. No single vaccine protects against all forms of HPV. The two most common HPV vaccines are the HPV-6/11/16/18 vaccine (Gardasil®) and the HPV-16/18 AS04-adjuvanted vaccine (Cervarix®).
The HPV-6/11/16/18 vaccine is designed to protect against HPV types 6, 11, 16, and 18.13 The HPV-16/18 AS04-adjuvanted vaccine protects against HPV types 16 and 18.14
Anyone up to age 45 and as young as nine can receive the HPV vaccine, although 11-13 is the suggested age range in the United States.15 The vaccine is given to both boys and girls, usually in two doses. Three doses are recommended for those with autoimmune disease.16
There is evidence, however, that the vaccine may be related to the onset of autoimmune disease including celiac disease, Addison’s, Hashimoto’s, and Raynaud’s, among others.17
One reason for this may be molecular mimicry between the vaccine and myelin basic protein, a component of the nervous system.18
This means that your body may attack its own cells after you have the vaccine because it can’t tell the difference between the proteins in certain cells in your body and the protein used in the HPV vaccine.19
Go Deeper
There’s an important relationship between molecular mimicry and autoimmune disease.
The Issues to Consider
There are four main takeaways you should be aware of:
- Those with autoimmunity may be more likely to contract HPV, including the varieties that cause cancer.
- Those who contract HPV may be more likely to develop an autoimmune disease such as lupus.
- The vaccine can prevent the strains of HPV that cause cancer.
- The vaccine itself has been linked to the onset of autoimmunity.
What Should You Do?
Testing for HPV
You should get tested if you do think you are at risk or might even have the virus.
Conventional doctors don’t generally test for HPV alone. Instead, they commonly perform a pap test to check for cervical cancer,20 which can arise from an HPV infection. I do recommend an annual pap test, regardless of your risk for autoimmunity or HPV.
There is a combination of HPV/pap; however, that’s rarely used. In functional medicine, we test for HPV much more frequently because the virus can be the root cause of other issues.
Evaluate the Risks
Remember, because the infection can lie dormant for so long, it’s possible to transmit HPV even years after exposure. Evaluating your personal risk will depend on your situation and your sex life, or those of your child long before she or he is sexually active. If you think they or you are at risk or might even have the virus, get tested.
Protect Yourself
Whether or not you opt for one of the vaccines, protect yourself from exposure. If you are not already in a long-term relationship with someone you trust who is HPV-negative, use condoms the right way, EVERY TIME. Use dental dams for oral sex, which come in various colors, flavors, and designs. Birth control pills will not prevent HPV and have actually been linked to a higher risk of cervical cancer.21
Support Your Immune System
Finally, support your immune system and detox pathways. Even if you do contract the HPV virus, an optimally-functioning immune system with fully functioning detox pathways can keep you from developing symptoms and the inflammation that can lead to further illness.
Methylation is a biochemical process that, among many other critical functions, transforms toxins into safer substances that will not harm your body. Methylation depends on a number of vitamins and cofactors, including folate, vitamin B12, and vitamin B6. Low levels of these three vitamins, in particular, have been linked to the progression of HPV infections in those who contracted the virus.
Those who have a heavy viral load and those with MTHFR gene mutations are particularly in need of support in their methylation process. The more mutations one has at this gene, the less able one is to make this conversion.
I personally have two gene MTHFR gene mutations. My Methylation Support formula is the perfect blend of the nutrients your body needs to engage in optimal methylation. I custom-selected these nutrients in their most bioavailable forms to support the body’s methylation and detoxification efforts.

Article Sources
- https://www.lupus.org/resources/lupus-facts-and-statistics#:~:text=The%20Lupus%20Foundation%20of%20America,living%20with%20lupus%20are%20women..
- https://familydoctor.org/condition/genital-warts/.
- https://www.who.int/news-room/fact-sheets/detail/human-papillomavirus-(hpv)-and-cervical-cancer.
- https://www.who.int/news-room/fact-sheets/detail/human-papillomavirus-(hpv)-and-cervical-cancer.
- https://obgyn.onlin.
- https://www.sciencedirect.com/science/article/pii/S0896841116302141.
- https://www.managedhealthcareexecutive.com/article/study-evaluates-possible-link-between-hpv-vaccine-autoimmune-disorders.
- https://presse.inserm.fr/en/human-papillomavirus-linked-to-auto-immune-disease/16322/.
- https://www.google.com/url?q=https://www.nova.edu/academic-affairs/faculty-research-grant/winners1011/human-papilloma-virus.html&sa=D&ust=1603819468154000&usg=AOvVaw0mItCAzYJsJye1YKgL-kxz.
- https://www.lupus.org/resources/understanding-the-hpv-vaccine.
- https://www.webmd.com/a-to-z-guides/autoimmune-diseases.
- https://www.mdedge.com/familymedicine/article/29595/infectious-diseases/sle-tied-higher-risk-hpv-infection.
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4641443/.
- https://www.ema.europa.eu/en/documents/product-information/cervarix-epar-product-information_en.pdf.
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4652326/.
- https://www.immunize.org/askexperts/experts_hpv.asp#disease.
- https://www.ncbi.nlm.nih.gov/pubmed/29044769.
- https://www.medsafe.govt.nz/committees/marc/reports/163-Gardasil-and-autoimmune-diseases.pdf.
- https://www.mayoclinic.org/diseases-conditions/multiple-sclerosis/expert-answers/demyelinating-disease/faq-20058521.
- https://www.glamour.com/story/why-arent-doctors-giving-more-young-women-hpv-tests.
- https://pubmed.ncbi.nlm.nih.gov/11943255/.
