Now, more than ever, it’s important to support those with celiac disease AND anyone with a gluten intolerance or sensitivity. That’s because the prevalence of celiac disease and gluten intolerance or sensitivity has increased significantly over the last 50 years.
I want to explain exactly what happens in your body when you eat gluten. This information is critical for those of you with celiac disease symptoms as well as those with gluten intolerance or leaky gut. Trust me when I tell you, even “just a little bit” of it can affect your health!
What Is Gluten?
Gluten (from Latin, “glue”) is a protein found in wheat that’s made up of the peptides gliadin and glutenin. It is also found in many other grains such as semolina, spelt, kamut, rye, and barley.
This protein gives bread its airy, fluffy texture and dough its sticky feel. It’s also used as a stabilizing agent in many processed foods including such surprising products as salad dressings and chocolate bars. It’s in almost everything from beauty products to packaged foods to medications and supplements. Even items labeled gluten-free can be cross-contaminated, so it’s best to avoid packaged foods as much as possible.
Is There a Difference Between Gluten Intolerance, Gluten Sensitivity, and Celiac Disease?
Before I describe what happens to your gut on gluten and what a leaky gut is, let me quickly define these terms for you. Gluten Intolerance and sensitivity are often used interchangeably, however, some consider a sensitivity to be a milder form of an intolerance. In either condition, consuming gluten leads to inflammation and uncomfortable symptoms including bloating, diarrhea, and pain. In the long term, it can also lead to leaky gut and inflammation anywhere in the body.
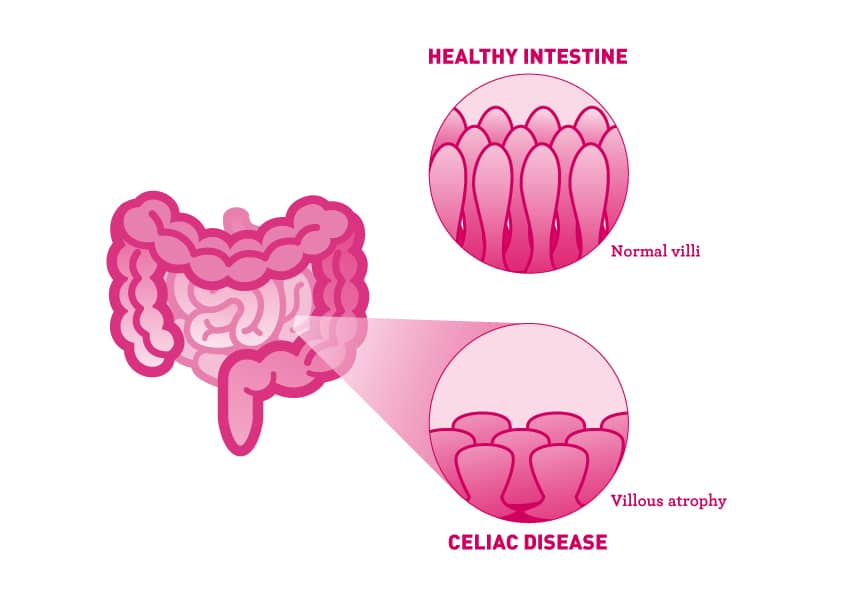
Celiac disease is a serious autoimmune disease that tends to run in families. In people who have it, any gluten they eat damages the villi in their gut, causing nutrient deficiencies. Those who are diagnosed with celiac disease are at risk of developing another autoimmune disorder.
 Dr. Amy Myers
May 15th, 2020
https://content.amymyersmd.com/article/leaky-gut-gluten-intolerance-celiac-disease/Illustrating the Normal Villi in a healthy small intestine vs. the villous atrophy and shortened villi from Celiac Disease – Infographic – Amy Myers MD®
Dr. Amy Myers
May 15th, 2020
https://content.amymyersmd.com/article/leaky-gut-gluten-intolerance-celiac-disease/Illustrating the Normal Villi in a healthy small intestine vs. the villous atrophy and shortened villi from Celiac Disease – Infographic – Amy Myers MD®Why Is Gluten Intolerance and Celiac Disease Such a Big Deal Now?
A 2009 study published in Gastroenterology showed that celiac disease has increased from one in 650 people to one in 120 people over the last 50 years.1 Some studies suggest that up to 30% of the population now suffers from gluten sensitivity.
What’s worse, an estimated 99% of people with celiac disease or gluten sensitivity are never diagnosed. More of us than ever are being negatively affected by this protein, yet most of us don’t know it.
We’re no longer eating the wheat that our parents ate. To have the drought-resistant, bug-resistant, and faster-growing wheat that we have today, we have hybridized the grain. It’s estimated that 5 percent of the proteins found in hybridized wheat are new proteins that were not found in either of the original wheat plants.2
These “new proteins” are part of the problem that has led to increased systemic inflammation, widespread gluten intolerance, and higher rates of celiac disease.3
Today’s wheat has also been deamidated,4 which allows it to be water-soluble and capable of being mixed into virtually every kind of packaged food. This deamidation has been shown to produce a significant immune response in many people.5 Lastly, in our modern fast-paced world with fast food at our fingertips, we are eating much more wheat than our ancestors ever did.
What Happens to Your Gut When You Eat Gluten?
Whether you are eating a sugary, fried doughnut or organic, 12-grain bread, the effects of gluten on your gut are the same. When your meal reaches your intestines, tissue transglutaminase (tTG), an enzyme produced in your intestinal wall, breaks down the gluten into its protein building blocks, gliadin, and glutenin.
As these proteins make their way through your digestive system, your immune system in your gut, the gut-associated lymphoid tissue (GALT), reviews them for potentially harmful substances. In people who have no issues with gluten, the proteins are absorbed.
In those with intolerance or sensitivity, the GALT identifies gliadin as a dangerous substance and produces antibodies to attack it. In celiac’s, these antibodies don’t just attack the gliadin, they attack the tTG as well, which is what originally broke down the gluten into its two parts.
This enzyme, tTG, has a number of jobs, including holding together the microvilli in our gut. Your body collects nutrients by absorbing them through the walls of your intestines, and the more surface area there is, the more they can absorb. Imagine trying to soak up a gallon of water with a paper towel versus a bath towel. Microvilli, which look like hairy fingers, exist in your intestines to increase the surface area and absorb nutrients.
When the antibodies your body produced to defend itself against gliadin attack your tTG, these microvilli can atrophy and erode, decreasing your ability to absorb nutrients and allowing the walls of your intestines to become leaky. This can manifest itself in digestive symptoms, including bloating, constipation, diarrhea, weight loss, fat malabsorption, and malnutrition, such as iron deficiency or anemia, low vitamin D, or even osteoporosis. This blunting of the microvilli is the hallmark of celiac disease.
Can Gluten Cause Leaky Gut Syndrome?
Regulating intestinal permeability is one of the basic functions of the cells that line the intestinal wall. In sensitive people, gluten can cause the gut cells to release zonulin, a protein that can break apart the tight junctions holding your intestines together.
Once these tight junctions get broken apart, your gut is considered to be leaky. A leaky gut allows toxins, microbes, undigested food particles, and antibodies to escape from your intestines and travel throughout your body via your bloodstream. The antibodies that escape are the ones that your body produced to attack the gliadin in the first place.
What Is the Link Between Gluten, Systemic Inflammation, and Autoimmune Disease?
Unfortunately, these antibodies often confuse more than just tTG for gliadin and end up attacking other organs and systems, from the skin to the thyroid to the brain. This is why gluten sensitivity is frequently paired with autoimmune conditions and why those with celiac disease are at risk of developing a second autoimmune disease.
I would suggest that if you have an autoimmune disease you get tested for gluten sensitivity, and if you’re found positive, you should get screened for autoimmunity.
How Do You Determine if You Have Gluten Intolerance?
The single best way is to go completely gluten-free for 30 days, then reintroduce it. Your body knows better than any test. If you feel significantly better when you’re not eating it or feel worse when you reintroduce it, then gluten is likely a problem for you, even if your lab tests are negative.
Lab testing for both is available as well, however, there are some inherent problems with this testing.6 Check out my article, “How to Test for Gluten Sensitivity and Celiac Disease,” for more information regarding this or purchase my Guide to Gluten eCourse.
What Should I do If I Have Gluten Sensitivity or Celiac Disease?
The only treatment is to eliminate gluten completely from your diet. However, you can still enjoy eating gluten-free grains such as quinoa, rice, wild rice, millet, and teff. Because trace amounts of gluten from cross-contamination or medications can be enough to cause an immune reaction in your body, skip any food that may be suspect. Concentrate your diet on naturally gluten-free foods such as organic fruits and vegetables as well as grass-fed beef and wild-caught fish.
When in doubt, go without. It’s simply not worth taking a chance.

For More Information
Thanks to a conversation I had with Dr. Tom Obryan, I learned how the subject of “non-celiac gluten sensitivity” has become so popular. Check out our conversation about how gluten appears in nearly everything we see in grocery stores today.
Article Sources
- //www.gastrojournal.org/article/S0016-5085(09)00523-X/abstract.
- https://www.ncbi.nlm.nih.gov/pubmed/20130747.
- https://www.ncbi.nlm.nih.gov/pubmed/11673371.
- https://www.ncbi.nlm.nih.gov/pubmed/11673371.
- //www.jacionline.org/article/S0091-6749(03)70089-X/abstract.
- https://consults.blogs.nytimes.com/2010/01/12/confirming-a-diagnosis-of-celiac-disease/?_r=1.
